
Analytics dashboards built to empower clinical and operational care teams
Arcadia Vista makes data more accessible with self-service dashboards that turn insights into enterprise-wide performance, faster — download the info sheet.
Retrofitting a business intelligence tool doesn’t work for healthcare
Business intelligence tools retrofitted for healthcare force data analysts to build bespoke and ad hoc reports for executives making critical decisions. Without a data model and reporting designed for the nuances of healthcare, trends can be missed, misunderstood across the organization, or discovered too late to influence change.
Success in the dynamic world of healthcare requires an in-depth and shared understanding of performance across a complex organization.
Use a software purpose-built for healthcare business intelligence
Arcadia Vista makes data more accessible by providing self-service dashboards — built in partnership with value-based care and healthcare pioneers — to turn insights into enterprise-wide performance, faster.
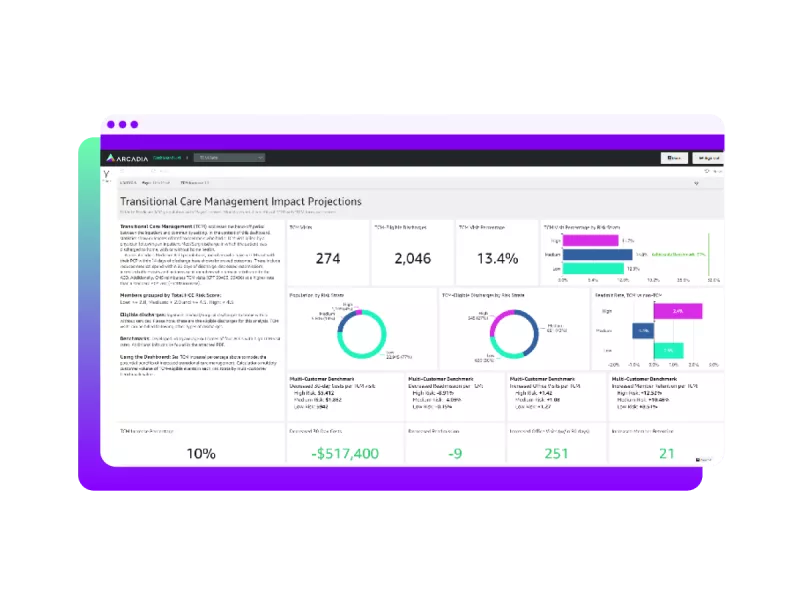
A direct path to sustainable growth
Analysts and leaders interact with Arcadia Vista’s growing library of healthcare intelligence dashboards — built on top of a data platform purpose-built for healthcare — to help data-driven leaders understand holistic performance and fine-grain detail.

Empower data-driven decisions and innovations in healthcare organizations

Understand your healthcare data to uncover deeper and actionable insights, faster

Understand what’s truly happening and optimize performance across the enterprise
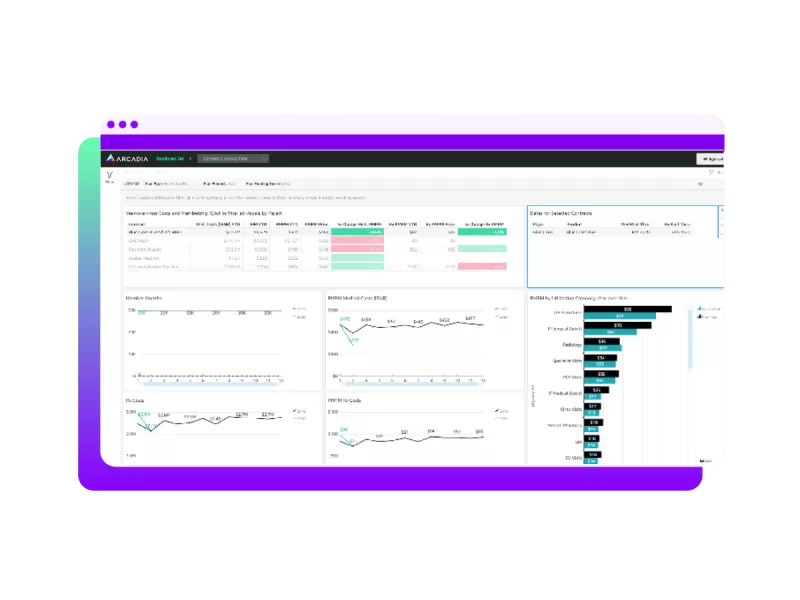
Your healthcare data has a story to tell
- Secure, web-based platform with interactive visualizations
- In-memory calculation engine for blazing fast response times
- Data discovery to empower healthcare analysts and users
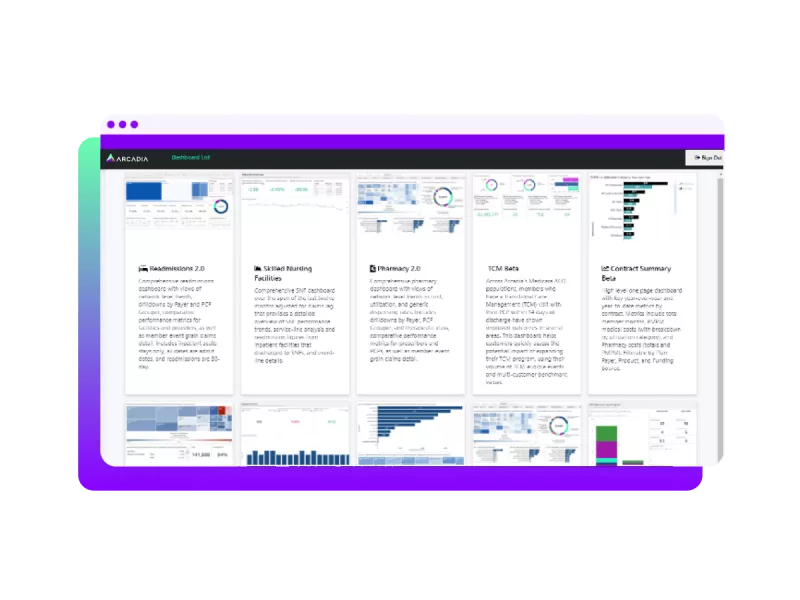
Growing library of business intelligence analytic content built for healthcare
- Leverage a growing, best-practice dashboards from a community of healthcare pioneers
- Analyses range from holistic contract management to detailed ROI projections for specific lines of business

Simplified and secure distribution of data insights
- Row-level security ensures data consumers see the appropriate data sets and populations
- Secure, in-app sharing of dashboards saves data analysts time and resources
- Arcadia Vista is built in collaboration with Amazon Web Services (AWS) on the QuickSight platform
We use the data that we can get from our claims to measure quality outcomes for our provider network. We measure quality improvement, and we leverage our claims-based data with our clinical data for providers to track quality outcomes. In the past, we have had some issues with data integrity and being able to reliably report quality outcomes. When we implemented Arcadia Analytics, all of that went away because we were able to trust the platform again. We have access to the raw data and can recreate the metrics so that we can do our own quality validation of the data. So we are able to go in front of our providers and demonstrate that we have good, clean data. From what we have seen and the feedback that we have received from those that are using the platform, there is a lot of potential for value.
Turn your healthcare data insights into performance improvements
Request a demo to see Arcadia Vista in action.
