
Data-driven care management to reduce healthcare risk and cost
Arcadia Care Manager enables comprehensive care management — download product info.
Large workloads spread care managers thin
Care managers have large caseloads that make it difficult to identify patients for care management programs and efficiently manage the tasks and events of the patient’s care plan. Disparate EHRs prevent care team members from seeing a complete view of a patient’s care plan and associated care team tasks. Missed patient identification or tasks can negatively affect an organization’s care coordination, quality of care provided, and total cost of care.
There’s a more efficient way.
Simplify care management with data-driven tools
Arcadia Care Manager utilizes predictive risk models, automated workflows, and insights from Arcadia’s comprehensive, longitudinal patient data set that result in efficient caseload management, improved care collaboration, and minimized risk. AI-enabled predictive risk models and best practices in workflows help care management teams scale their programs through simplified processes, more care collaboration and focus that reduces risk and cost.
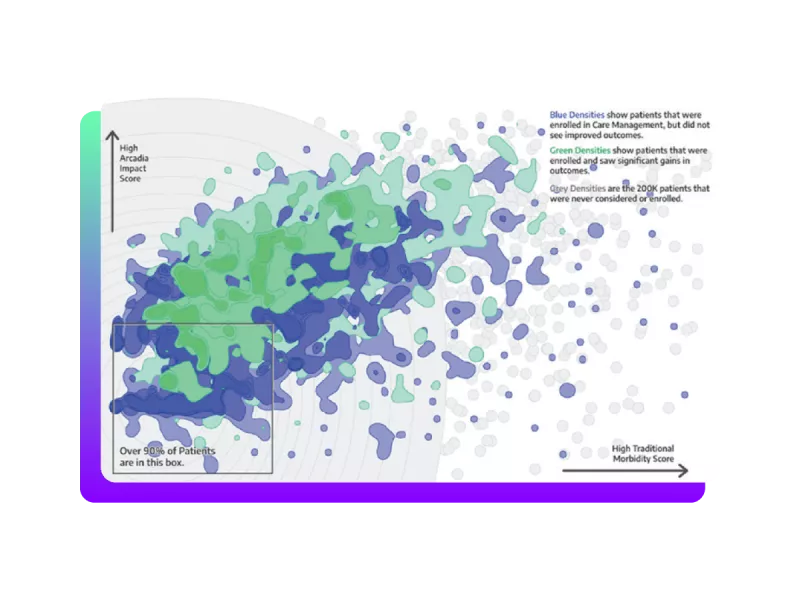
Create clinically-relevant care programs at scale
- Leverage risk models that utilize a comprehensive, longitudinal view of the patient
- Reduce barriers to quick usage and increase time to value with preconfigured workflows
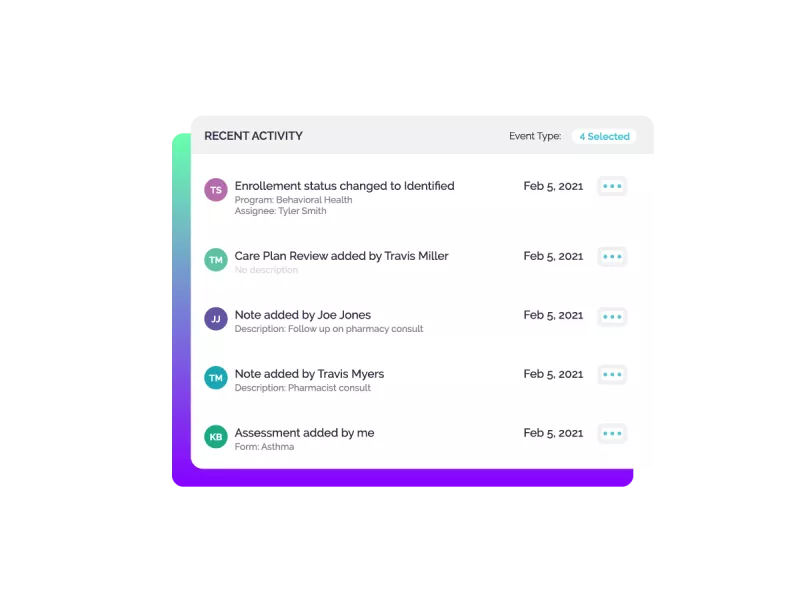
Improve care coordination and collaboration
- Access comprehensive patient information, no matter where the information lives
- Facilitate collaboration among team members with shared workflows, care plans, and tasks
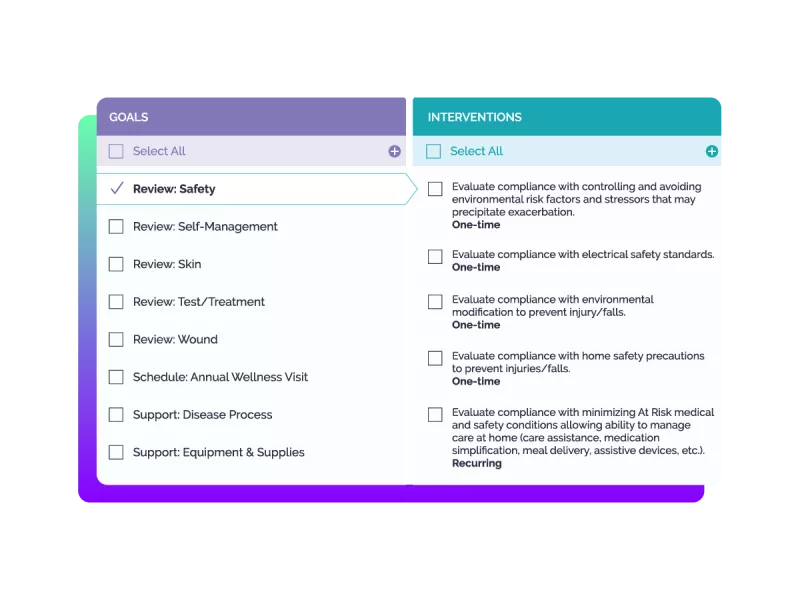
Increase time care managers spend on high-value activities
- Efficiently create and manage large care programs
- Leverage preconfigured content, developed with leading healthcare-focused, evidence based content experts, MCG and Eventium
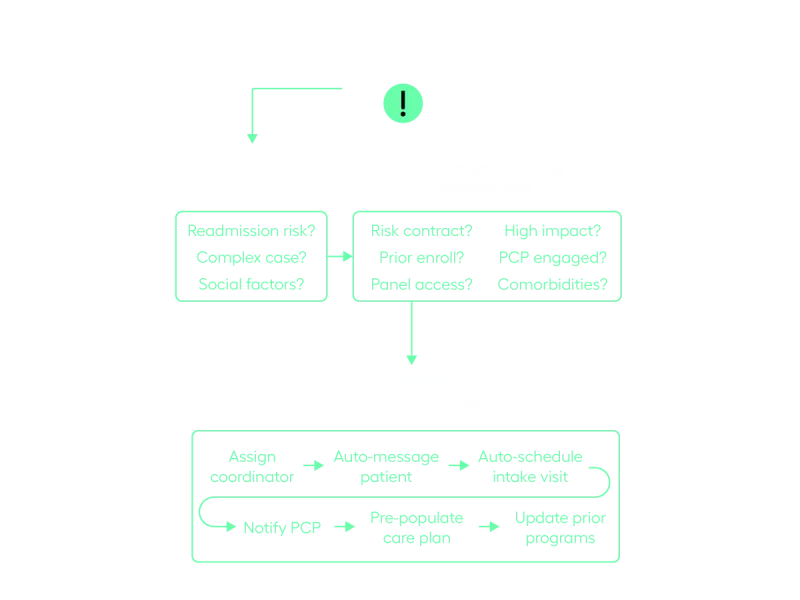
Real-time decision making, program routing, and process automation
Automate decision-making and time consuming processes to enable your staff to focus on high-value tasks. When a patient is discharged, the system triggers the case enrichment algorithm. This algorithm checks against the care program routing decision tree and generates, checks, and executes on automated tasks — all without human intervention.
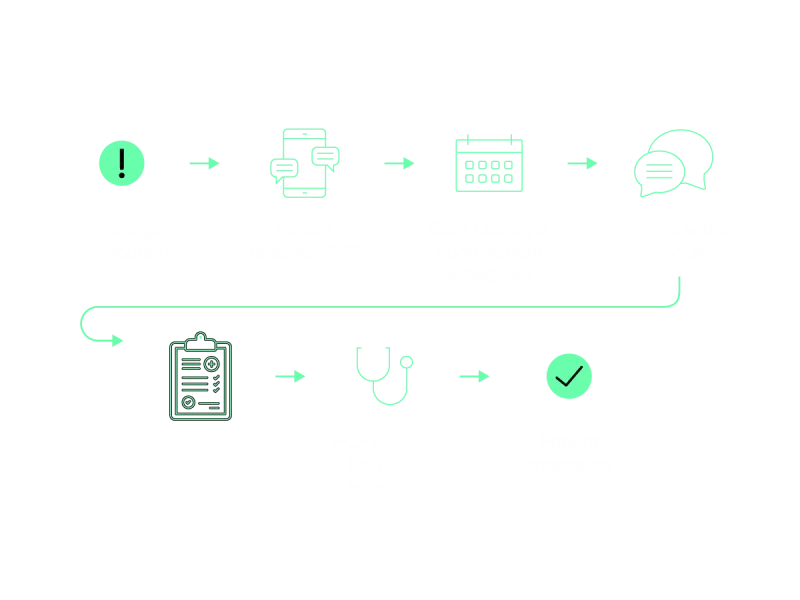
Seamless patient routing and task management across apps — available through Arcadia Engage
Combine Arcadia Care Manager with our patient engagement tool, Arcadia Engage, to automatically set up the patient’s follow-up. On discharge the patient receives text messages and a care manager appointment is scheduled to call within 48 hours. The care plan is automatically populated and the primary care physician is notified for the seven-day follow up.
There are options we like from Arcadia. We like the data that has been made available. We have clinical data, claims data, and ADT data all put together in the system. We like how easy the system is to use for end users. We also like being able to save reports and create shortcuts for users. Arcadia keeps up with industry trends and has new functionalities available.
Improve and scale your care management teams
Request a demo of Arcadia Care Manager to see other use cases.
